A Brief Colonial History Of Ceylon(SriLanka)
Sri Lanka: One Island Two Nations
A Brief Colonial History Of Ceylon(SriLanka)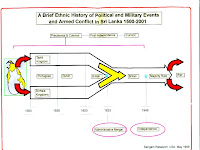
Sri Lanka: One Island Two Nations
(Full Story)
Search This Blog
Back to 500BC.
==========================
Thiranjala Weerasinghe sj.- One Island Two Nations
?????????????????????????????????????????????????Saturday, November 28, 2015
How Liberia’s Latest Ebola Case Slipped Through the Cracks
Just
weeks after the country was declared Ebola free, the newest case of the
deadly virus revealed worrying shortfalls in its ability to prevent
another outbreak.

It was like a story from the early days of the Ebola epidemic.
Fifteen-year-old Nathan Gbotoe was weak and bleeding from the mouth,
traveling with his father and four other people in a neighbor’s car from
a crowded clinic, seeking treatment. Finally Gbotoe ended up at John F.
Kennedy Medical Center, Liberia’s largest public hospital, located in
the heart of the capital, Monrovia. His father claimed his son had been
cut during an accident. His temperature was checked and he didn’t have a
fever — none of the health workers responsible for triaging patients
suspected him of being infected with the virus. Unable to walk, Gbotoe’s
father pushed him in a wheelchair to the trauma ward. A nurse wearing
her everyday scrubs pulled on latex gloves and examined the inside of
Gbotoe’s bleeding mouth. Finding no cut, she sent him to the children’s
emergency ward. Two days later, doctors tested him for Ebola. When it
came back positive a few hours later, he was taken to an Ebola treatment
unit. Three days after that, he was dead.
Gbotoe’s case, which was announced on Nov. 20, put an end to Liberia’s official “Ebola free” designation for a second time this year — doing so days after Guinea discharged its last patient and
Sierra Leone counted its second week without a known case of the virus.
While the source of Gbotoe’s infection is currently being investigated,
the mismanagement of his case at the nation’s largest public hospital
raises questions about Liberia’s preparedness to handle future
outbreaks.
What went wrong? Seemingly a lot.
Gbotoe should have been fully checked by a triage at the entrance at the
hospital where health workers screen for patients who may have Ebola
and need to be isolated. The doctors and nurses who handled his case
didn’t wear the correct equipment for treating possible Ebola cases that
protects against the highly infectious virus. Dr. Mosoka Fallah, the
leader of the outbreak response who traced most of the cases through
Monrovia and Liberia during the heat of the outbreak, said there was an
overreliance in medical facilities on fever being an indicator of
possible infection.
“There should be a high level of suspicion because 90 percent of the
patients lie,” said Fallah. In other words, Gbotoe should never have
slipped through the cracks.
Still, Dr. Francis Kateh, the chief medical officer and acting head of
the Incidence Management System that manages Ebola cases, denied there
had been a breach of protocol. “No one would walk around with full
[personal protective equipment] in this climate,” he said over the
phone. After the initial lapse, the official mechanism for dealing with
an outbreak clicked on. The nine medical workers who came into contact
with Gbotoe are now quarantined and 152 contacts have been identified,
among them patients and health workers, according to Kateh. Tracers who
monitor all the people that have been in contact with the Ebola patient,
should they become symptomatic, are still looking for 18 persons. “They
are trying to evade us and avoid our calls, it is very concerning,”
Fallah said.
The children’s emergency ward at the hospital has been decontaminated
and remains closed, the patients discharged to their home and currently
under observation. The nurse who examined Gbotoe in the trauma unit has
been quarantined, but the ward itself has not been decontaminated.
According to a worker at the hospital, Gbotoe only spent a very short
amount of time in the ward.
The late Gbotoe’s 8-year-old brother and father also contracted the
virus but remain in a stable condition, along with his mother and his
two young siblings. All are receiving Zmapp — an experimental medication
for Ebola — for treatment, according to a report by the Ministry of
Health. After they were removed from their home on Thursday night, Nov.
19, a spray team came in later the following day and finally
decontaminated the house.
What is so worrisome about Gbotoe’s case, however, is that what should
have been obvious red flags went uninvestigated for critical days. Since
the darkest days of the epidemic, which claimed the lives more than
11,000 people throughout the region — including many doctors and nurses
at hospitals such as John F. Kennedy — the World Health Organization,
and other NGOs have conducted mass trainings of
medical workers in identifying the symptoms of the virus and the
precautions needed when handling a suspected Ebola case. Bleeding is
uniquely associated with Ebola and Lassa fever, a common virus in West
Africa, but was not as typical among
Ebola patients during the West African outbreak that started in
December 2013 as it has been in previous outbreaks. Other more common
symptoms of the virus such as diarrhea, fever, nausea, and vomiting are
linked to diseases that are endemic to the region such as malaria,
typhoid, and cholera, and make the virus more difficult to detect.
A worker at the Ebola unit where Gbotoe was being treated until his
death, who wished to go unnamed because of fear of punishment, expressed
amazement that the case had initially gone unnoticed.“You think that
they would have picked it up, that it would be obvious by now,” the
worker said.
The questions raised by the case go beyond how it was handled, underscoring concern about how little is known about its origins.
In an attempt to shed light on this, scientists from the United States
Army Medical Research Institute of Infectious Diseases arrived in
Liberia on Monday, Nov. 23, to do genetic sequencing tests to determine
whether the new infections are linked to a previous chain of
transmission — a method that has been used over the past year to map out
the course of the epidemic in the region. In July, tests were done when
a mysterious case emerged in a community just outside of Monrovia, near
Liberia’s international airport. The body of 17-year-old Abraham
Memeigar tested positive to Ebola after a safe burial team dressed in
hazmat suits took a swab from his body. The case emerged just weeks
after Liberia was declared Ebola-free for the first time, on May 9.
Memeigar’s body was exhumed from the grave so that a blood sample could
be taken to gain more information about the chain of transmission. The
tests determined that the virus present in Memeigar’s body was connected
to the Ebola virus circulating in Liberia, rather than other strains in
Sierra Leone and in Guinea. Five others were infected. The origin of
the case was never determined.
Memeigar’s case was not detected until his death. The clinic that he
visited for treatment did not raise the alarm, but rather sent him home
with malaria medication. Memeigar’s infection, like Gbotoe’s, was not
detected by community members or health workers. A woman who was
connected to Memeigar’s case was later quarantined and died.
“The fact that we picked it up means the system is working,” said Peter
Graaf, the head of the United Nations Mission for Emergency Ebola
Response at the time of the outbreak (UNMEER has since been dissolved).
“Unfortunately not every case is handled this way. In a sense we got
lucky.… So it is a bit of a wakeup call.” Experts are now concerned that
that wakeup call didn’t quite ring loud enough.
Memeigar’s case similarly raised concerns about basic infection
prevention and control in health clinics and hospitals in Liberia.
“While ‘post-Ebola’ planning has focused on long-term aspirations, the
very gaps in basic infection control that facilitated the epidemic’s
growth in the first place have still not been addressed,” said Aitor
Sanchez-Lacomba, the director of the International Rescue Committee in
Liberia, after the Memeigar case was discovered. “These include having
water, sanitation, and basic equipment at facilities; ongoing community
surveillance; and triage procedures adapted not only for Ebola, but
other epidemic diseases.”
The emergence of these two small outbreaks call into question more than
the preparedness of health workers on the ground; they also cast doubt
on the World Health Organization’s classification of countries as
Ebola-free after they pass 42 days without a case. They also call into
question scientific understanding of how the virus works. Fallah said
Gbotoe’s mother “may have been a survivor” — a lead that investigators
appear to be pursuing to explain the current outbreak. Research projects
have been launched that explore the causes of outbreaks and nature of
the virus, which will lead to a greater understanding of how it can be
prevented. In June,
the National Institute of Health began a study into survivors,
investigating the health problems they experience, their immunity, and
how long the virus can remain in the semen. A recent report by
the Environmental Foundation for Africa looked at the how potential
threat of viruses like Ebola will grow as humans continue to encroach on
local wildlife and a comprehensive study into the role that
encroachment on the human environment may be playing in Ebola outbreaks
will soon begin.
“On one level, the 42-day approach makes a lot of sense given what we
know, but if these flare-ups reoccur we may need to reassess it,” Ashish
K. Jha, director of the Harvard Global Health Institute said in an
interview. “Being Ebola-free forever may not be a realistic goal.”
Jha was part of an independent panel of 19 experts who released a reportpublished in The Lancet on
Nov. 22 that slammed the World Health Organization for its slow
response and made a series of recommendations on how to improve both the
global and domestic responses to outbreaks of disease in these
countries. The report called on the global community to develop a “clear
strategy” to ensure that the governments of Sierra Leone, Liberia, and
Guinea invest in detecting, reporting, and responding to outbreaks. It
also called for greater international support to these countries,
including greater resources to rebuilding health care systems coupled
with a “transparent central system for tracking and monitoring the
results of these resource flows.”
Liberia’s Ministry of Health has developed a 7-year, $1.7 billion plan
to revitalize the country’s health system. The first two years of the
plan — which will involve training of health workers, remodeling health
infrastructure, and improving emergency preparedness and response — will
require $400 million of funding according to the minister of health,
Dr. Bernice Dahn. While international donors have shown more of an
interest in funding the health care system it is unclear whether many of
them are committed for the long haul. The first two years are yet to be
fully funded.
As the country begins to move past the Ebola nightmare, however,
Gbotoe’s case is a fresh warning of how much still needs to be done. “We
are better prepared than we were two years ago, but are we where are
not where we need to be, not even close,” said Jha.
ZOOM DOSSO/AFP/Getty Images

